The College that works.
Your future starts here. At The New York School for Medical and Dental Assistants we'll support you every step of the way as you train for a rewarding career in Medical Assisting, Dental Assisting, and more. Let us help you achieve your career goals.
Medical assistant programs New York NY
Learn more on our Privacy Policy here
Look where our graduates are working


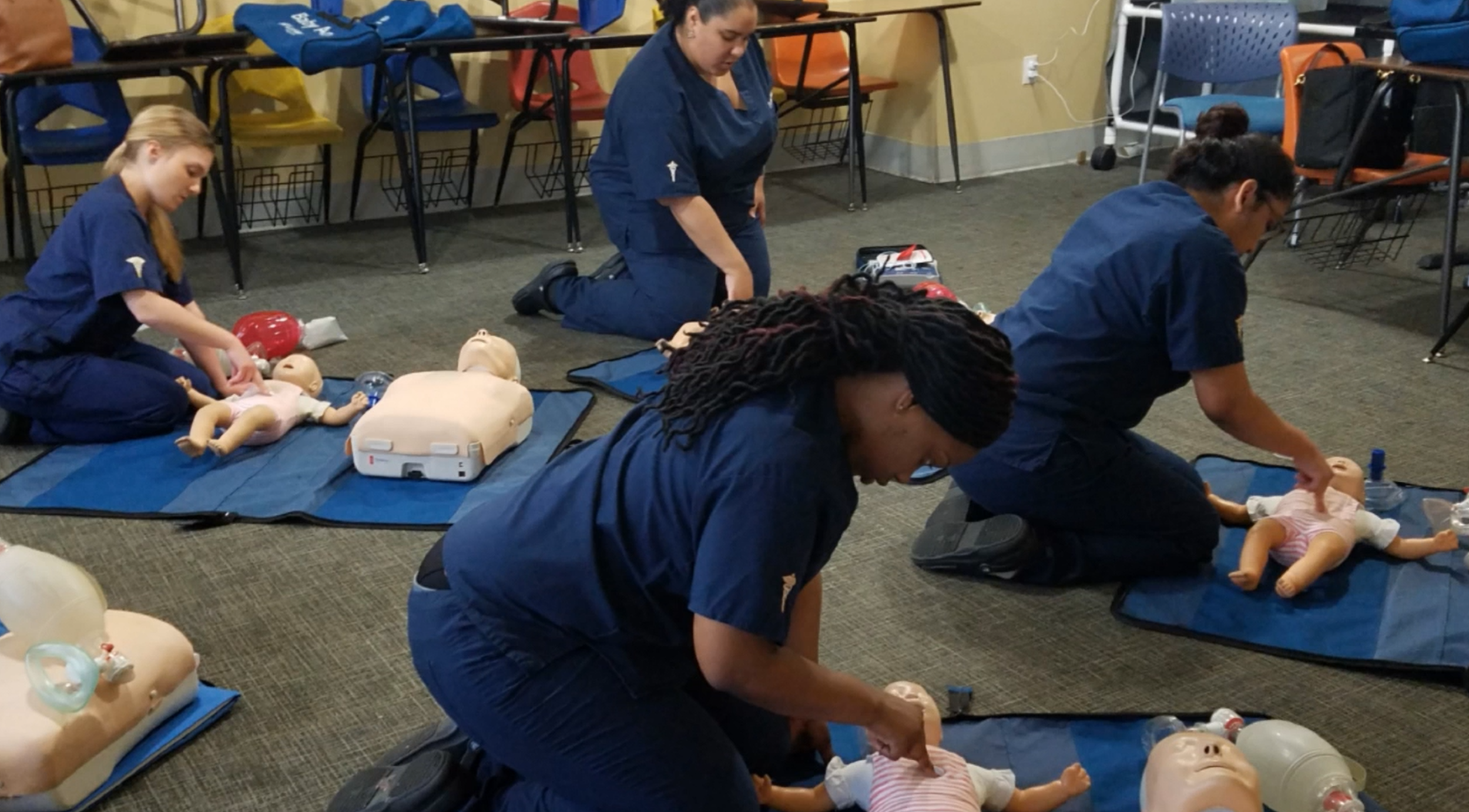
Step right up and discover what we bring to the table at The New York Dental and Medical Assistant School New York! From mastering the art of patient care to juggling dental tools with flair, there's so much to learn here. Our curriculum is sprinkled with a dash of uniqueness that sets us apart.
NYSMDA Training Programs

Step into a world where stethoscopes meet smiles! We're not just teaching skills; we’re crafting future medical and dental wizards. It’s a fun ride filled with hands-on experience and plenty of inspiration.
Your story is waiting to unfold – let’s dive into the excitement together!
Who we are!

Get in touch with NYSMDA
Interested in learning more about the New York School for Medical and Dental Assistants? Fill out some info and we will be in touch shortly! We can't wait to hear from you!

Learn more on our Privacy Policy here